
Hearing allows us to do more than simply understand what is being spoken. From the moment of birth and throughout infancy, our sense of hearing is closely linked to speech and language development and even mild to moderate levels of hearing loss can lead to changes in the brain1. Hearing loss in babies has been called a “neurodevelopmental emergency.”2 The evidence-based research supports a very short critical time window of 6 months to realize the benefits of early experience with language and sound. A newborn’s inability to hear their linguistic environment will contribute to delays in language development and perhaps social, cognitive, and educational difficulties throughout their lifetime.
Significant permanent congenital hearing loss is one of the most common disorders present at birth worldwide, affecting 2-3 per 1000 births2. The importance of early detection and treatment of hearing impairment in a newborn has been studied extensively. Significant developmental delays have been identified with delayed diagnosis and treatment of infant hearing loss. Universal Newborn Hearing Screening (UNHS) is an essential practice to offer all newborns the opportunity for accurate and early diagnosis of hearing impairment. Healthcare systems should establish best practices for conducting newborn hearing screening using the most accurate and effective technology available.
Hearing Impairment is not a visible condition at birth, and the cause of newborn hearing loss can be elusive. Most children with congenital hearing loss are born to normal hearing parents and have no health issues or risk factors for hearing loss. A Belgian study3 shows that the origin of hearing loss can only be identified in half of children referred by hearing screening. Of these, 60% of hearing loss was congenital and 19% suffered from cytomegalovirus infection. Other common factors for a high risk of hearing loss include premature birth, ototoxic medications, hyperbilirubinemia, or syndromes associated with hearing loss such as Waardenburg or neurofibromatosis.
The high prevalence of congenital hearing loss suggests, however, that even an apparently healthy baby, with no risk factors might still be susceptible to hearing deficits. Therefore, every infant — even those who appear healthy in all respects — should receive a newborn hearing screen. Additionally, research supports the Early Hearing Detection and Intervention (EHDI) guidelines4 advocating that early intervention for hearing loss is initiated no later than six months of age. Therefore, early screening at birth is strongly recommended.
Since universal newborn hearing screening is encouraged and early screening is preferred, the only remaining question is how to prioritize infants and newborns for hearing screening. Timing is important — too late means missing the diagnosis and intervention window, and too early means potentially risking less accurate results or higher refer rates. For healthy newborns in the well-baby nursery, screening should be conducted within a narrow window, preferably before the newborn is discharged from the hospital but certainly before the infant reaches one month of age. For infants in the NICU, screenings should be completed when the infant is stable, out of an incubator, and healthy enough for hospital discharge.
Technological Considerations for Newborn Hearing Screeners
We have demonstrated that early hearing detection and intervention is necessary for the best social, emotional, and educational outcomes possible. The next step is to ensure all newborns undergo a hearing screening using fast, accurate, and minimally-invasive screening technology.
Technology choices for newborn hearing screening5 include evoked otoacoustic emissions (EOAE, commonly shortened to OAE) or auditory brainstem response (ABR). Using OAE for newborn screening involves placing a probe with a miniature microphone and speaker into the newborn’s ear canal to stimulate and measure responses from the cochlea within the inner ear. ABR screening involves placement of three small sensors on the infant’s head to measure brainwaves occurring in response to a soft click stimulus presented to the ear.
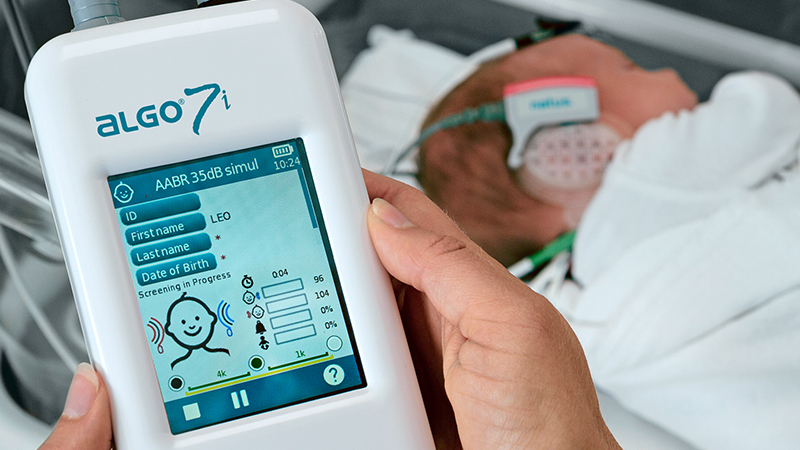
While both OAE and ABR screen for hearing impairment, the ABR screening is the only screening method that screens the entire auditory pathway, from the ear to the brain. Let’s take a closer look at the differences in these two technologies.
Otoacoustic emissions (OAE) are sounds created in the inner ear in response to a sound stimulus. A small probe containing a miniature speaker delivers a sound to the ear and a microphone within the probe measures the emission (acoustic response) coming back from the cochlea in the inner ear. Automated technology will score the response as a PASS or REFER.
The upside of OAE screening is that it is fast and inexpensive to perform. The screening may take only seconds with calm, quiet newborn. The OAE requires one single-use disposable eartip per screening, resulting in lower consumable cost for the screening program.
One primary disadvantage of OAE screening is the higher number of newborns who will not pass the screening. The OAE is very susceptible to moisture and vernix in the infant’s ear canal. OAE screenings conducted within the first day or two of life have a higher likelihood of referring due to the status of the infant’s ear canal and not at all related to the status of the infant’s hearing. These false positive results contribute to un-necessary parental anxiety and create additional workload for caregivers needing to perform additional screenings on a higher than expected number of infants who do not pass.
Perhaps the biggest disadvantage with OAE screening is that OAE screens only a portion of the hearing pathway, up to the level of the cochlea in the inner ear. While most congenital hearing impairments are due to problems in the inner ear, 15% or more are due to problems involving the auditory nerve, referred to as Auditory Neuropathy Spectrum Disorder or ANSD. Newborns with hearing deficits from an auditory nerve abnormality will pass on the OAE screening. False negative screening results lead to a delay in diagnosis and management.
In contrast to OAE screening, an Automated Auditory Brainstem Response or AABR screening requires a few minutes to prepare the infant for screening, and to measure the responses, but the AABR is a more complete screening of the entire auditory pathway. AABR screening is performed on an infant who is quiet and relaxed, preferably sleeping. In addition, most AABR screening technologies use disposable, single use only sensors and ear couplers, associated with a higher per-screening cost to the facility, if based on supplies cost alone.

Benefits of AABR include the ability to perform screenings as early as 6 hours of age, a lower refer rate, fewer re-screens, reduced loss to follow up and less parental anxiety. This means that there is less of a cost disadvantage than one might immediately assume, as fewer rescreens are required. This leads to less babies enrolled in follow up programs or leaving the hospital with an outpatient appointment for rescreening, therefore parents are less likely to miss any follow-up screening appointments if accurate and complete screening can be performed from the outset.
Lastly, and perhaps most importantly, AABR screening technology has the highest sensitivity (lowest false negatives) and highest specificity (lowest false positives)6 as compared to OAE screening. AABR screens the entire auditory pathway and can identify infants with hearing abnormalities within the cochlea and the auditory nerve.
Because of its advantages in terms of accuracy, sensitivity, and specificity7, an AABR hearing screen is the better tool for screening for newborn hearing deficits. Adding automation to traditional ABR has dramatically improved the technology, allowing for a more consistent, complete, objective test that eliminates operator bias and interpretation. AABR is less susceptible to interference from room noise, can be performed within hours of birth and simultaneous testing of both ears can be achieved. In short, AABR is the technology of choice when early, accurate and proven screening technology is a requirement.
For more information on Automated ABR and how to use it in your practice, download our white paper today.
Sources:
1. Heuser Hearing Institute (2019) Hearing Loss in Kids Can Affect Brain’s Sound Processing.
2. Karen L. Anderson, PhD (2011) Brain Development & Hearing Loss.
3. Luxon L.M (2014) Hearing Loss. Encyclopedia of the Neurological Sciences (second Edition) 2014, Pages 533-538.
4. Taylor J. A et al (2012) Hearing Screening. Avery’s Diseases of the Newborn (Ninth Edition),chapter 26.
5. Early Hearing, Detection and Intervention Program: A Program of the American Academy of Pediatrics.
6. Katarzyna E et al (2017) Universal newborn hearing screening: methods and results, obstacles, and benefits. Pediatr Res 81, 415–422 (2017).
7. Heidari S. et al (2015) The sensitivity and specificity of automated auditory brainstem response and otoacoustic emission in neonatal hearing screening: a systematic review. Aud Vest Res (2015);24(3):141-151.
8. Sena-Yoshinaga T.A et al (2014) Neonatal hearing screening with automated auditory brainstem response: using different technologies Audiol., Commun. Res. vol.19 no.1 São Paulo Jan./Mar. 2014
035112 RevA
